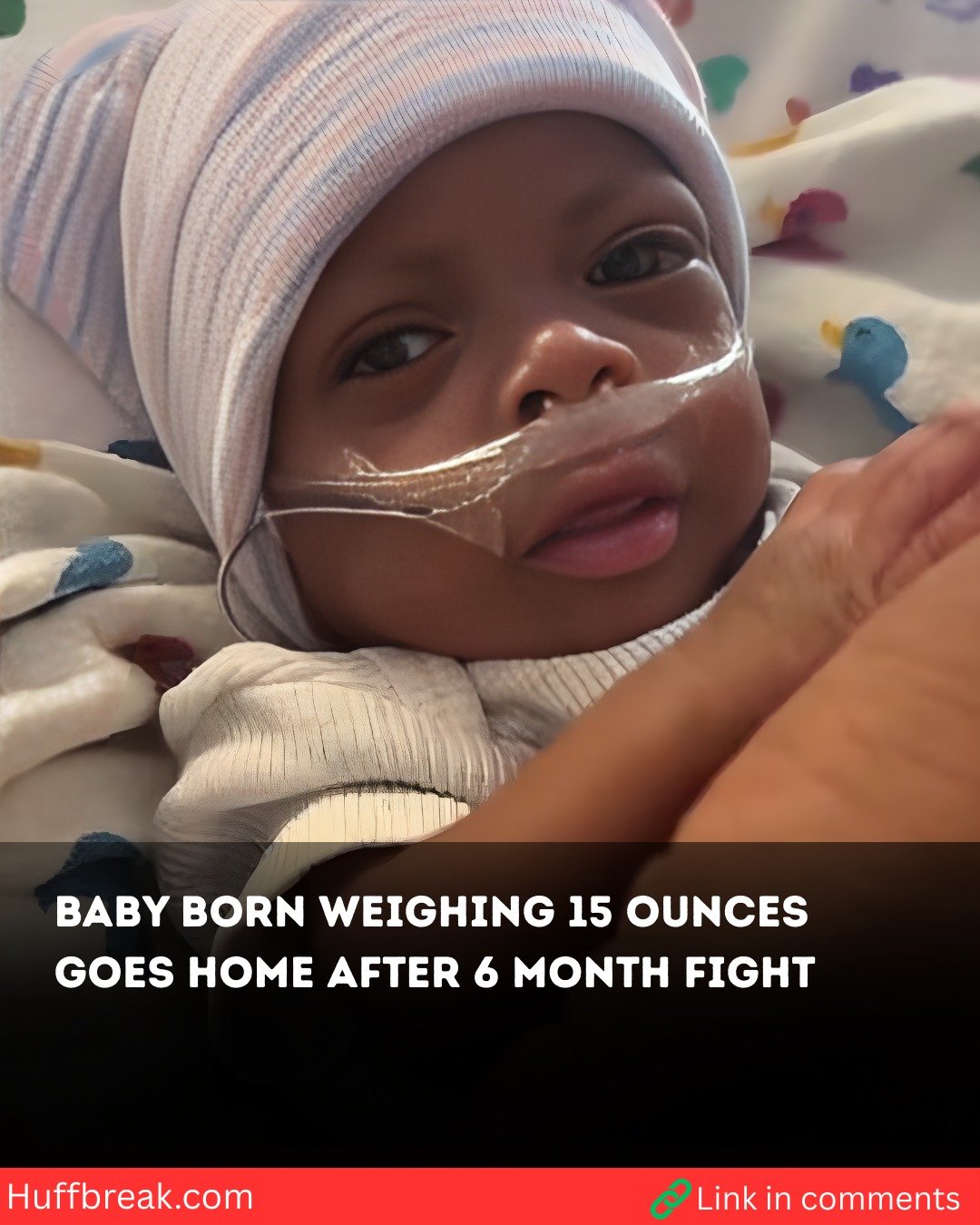
Labreshia Howard still remembers the day the room went quiet.
At a normal twenty-four-week check-up the doctor moved the probe, frowned, and said the sentence every mother fears: “I can’t find the heartbeat, and she’s far too small.”
In that moment the happy buzz from the pink-confetti gender reveal a few days earlier vanished, and Labreshia’s world shrank to the size of a shrinking baby.
Doctors at UT Health East Texas sprang into action, admitting her on the spot, hoping to keep the little girl safely tucked inside for just a few more priceless days.
Three tense days later the monitors screamed; it was time to deliver, ready or not.
When Addisyn slipped into the world she weighed only fifteen ounces—lighter than a can of Coke, smaller than the disposable diaper the nurses laid beside her like a blanket.
Her cry was no louder than a kitten’s, but it was proof she was alive and ready to fight.
The neonatal team swaddled her in plastic wrap to keep her thin skin from losing heat, slid the tiniest breathing tube into her mouth, and hooked her to machines that beeped and blinked like a spaceship cockpit.
Labreshia saw her daughter for only a few seconds before the incubator door closed and the NICU became their second home for half a year.
Every morning she walked the long hallway, pressed the silver button, scrubbed her hands raw, and whispered the same prayer: “Let her grow today.”
Grow she did, gram by stubborn gram.
Addisyn traded the ventilator for nasal prongs, the feeding tube for a tiny bottle, and the clear isolette for an open crib that looked enormous around her.
Nurses cheered when she hit one pound, then two, then three; each ounce was a trophy.
They fashioned doll-sized clothes from preemie outfits, turned surgical masks into festive hats for holidays, and pasted her footprints on a growth chart that started later than most but climbed just as surely.
Marcie Tunstall, the nursing director, says the whole women’s and children’s floor adopted the baby: “We celebrated her first bath, first sneeze, first yawn like she was our own.”
The hardest part for Labreshia was going home without her child.
Night after night she sat in the empty nursery, stared at the unused rocking chair, and texted the night-shift nurse for photos.
She learned the language of oxygen saturations, bradycardia spells, and fortified breast milk; she also learned patience, the quiet kind that whispers, “Tomorrow will be better.”
Dads, moms, grandparents, and even cafeteria workers began stopping by the NICU to see the “little fighter,” leaving behind encouraging sticky notes that covered the incubator like bright wallpaper.
Slowly the terrifying beeps became background music, and the ounces turned into pounds until one morning the doctors said the magic words: “She can go home.”
The send-off felt like a championship parade.
Nurses lined the corridor waving pink pom-poms, respiratory therapists held glittery signs, and lab techs blew bubbles that drifted over the rolling incubator like tiny moons.
Labreshia pushed the crib past the double doors, breathing hospital air for the last time, while Addisyn—now a plump five pounds—slept through the whole celebration under a crocheted blanket.
Bonnie Bearden, the clinical manager, calls every NICU parent a world champion, because watching your child fight for life and win is its own Olympic event.
Labreshia just smiles, kisses the top of her daughter’s head, and repeats the promise she made when Addisyn was still smaller than a Coke can: “You did the hard part, baby; now the rest of the world is yours to conquer.”