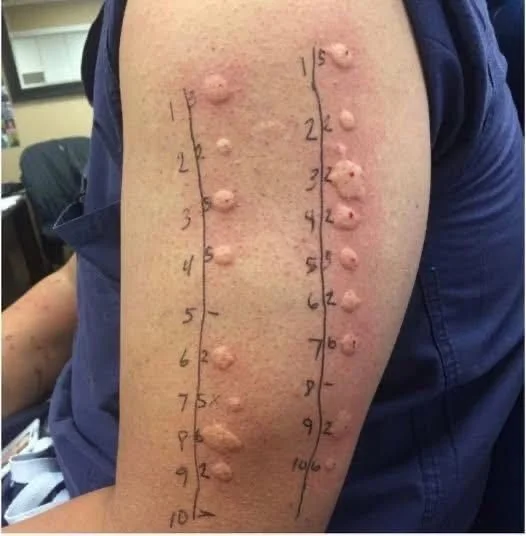
For James, it started as a minor distraction—a simple itch on his forearm. But this distraction soon grew into an all-consuming presence. The itch spread in a wave, moving to his legs and torso with a stubborn intensity that dominated his thoughts, especially in the quiet hours of the night. Sleep became fractured, and his days were clouded by fatigue. The arrival of red, raised welts was baffling; there was no new detergent, no strange food, no apparent reason. This was the beginning of a silent conversation where James’s skin was trying urgently to tell him something he couldn’t yet understand.
After weeks of ineffective self-treatment with drugstore remedies, James realized he needed a translator for his body’s cryptic signals. He made an appointment with a dermatologist, who listened carefully and examined his skin. The diagnosis was chronic urticaria, a form of hives that persists for weeks or months, often without a discoverable cause. In James’s case, it wasn’t an allergy to something external, but rather his own immune system behaving as if under constant, false alarm. This internal mix-up can be triggered by a host of subtle factors, from a past viral infection to stress, making it a complex puzzle to solve.
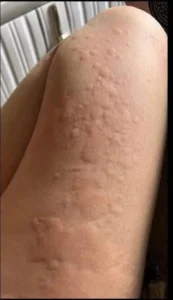
Receiving this diagnosis was a watershed moment. While chronic urticaria is not life-threatening, its impact on quality of life is profound. The relentless physical sensation, the sleep deprivation, and the self-consciousness about visible symptoms create a heavy emotional toll. For James, understanding that his condition was real, recognized by medicine, and shared by countless others lifted a veil of isolation. It transformed his struggle from a lonely, confusing battle into a manageable health challenge with defined strategies for care.
Management became James’s new focus. His treatment plan was two-fold: targeted prescription medications to dial down the immune system’s overreaction, and mindful lifestyle adjustments to reduce stress and support overall health. The combination worked. Gradually, the tormenting itch released its grip. He began to enjoy uninterrupted sleep again, and the fear of sudden flare-ups diminished. James found empowerment not in a magic cure, but in knowledge and a proactive plan. He was no longer just reacting to his skin; he was thoughtfully responding to his body’s needs.
This experience highlights a crucial truth: your skin is a powerful messenger. A persistent itch that disrupts your life is rarely just about the surface. It can be an early sign of internal dynamics, from immune function to other systemic health considerations. Ignoring these persistent signals means missing an opportunity for timely intervention and relief. If an itch lasts more than a few days, resists common treatments, or significantly interferes with your daily rhythm, it is a message worth heeding. Consulting a healthcare professional is the first step in turning that message into a roadmap for recovery, comfort, and reclaiming your peace of mind.